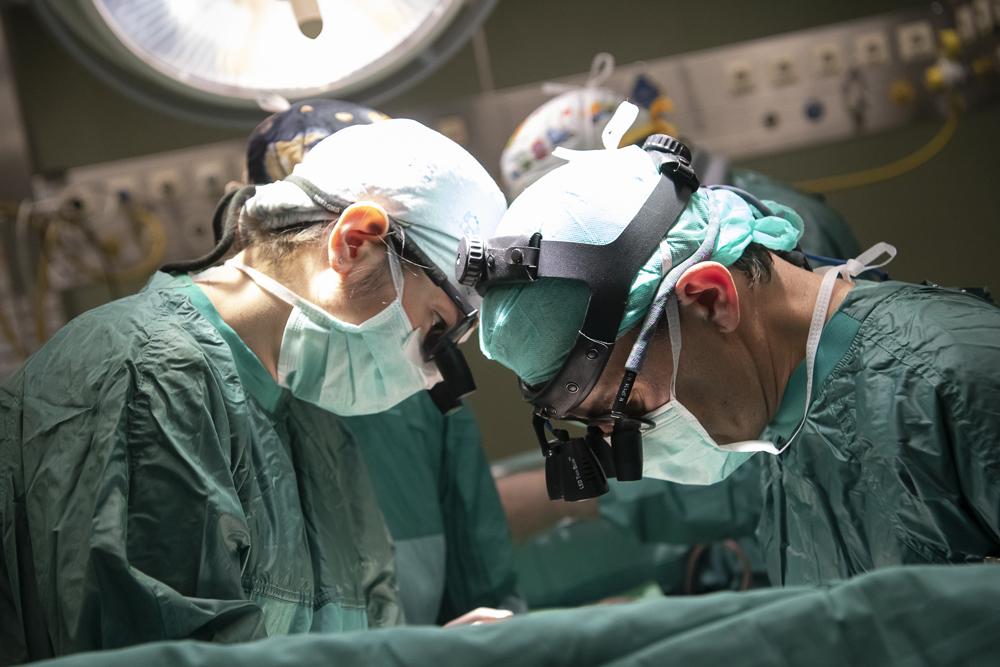
The combined kidney and liver transplantation is more effective than kidney transplant alone for treating patients with methylmalonic acidemia and renal failure caused by this rare metabolic disease. This is shown by a multicentric scientific study coordinated by the Bambino Gesù Children’s Hospital. The results already presented during the tenth congress of the International Pediatric Transplant Association (IPTA) will soon be published in an international scientific journal. “The conclusions of the study have very important repercussions on the transplant programs of many centers” explains Dr. Luca Dello Strologo, in charge of kidney transplantation follow-up at the Holy See Hospital.
METHYLMALONIC
ACIDEMIA
Methylmalonic acidemia is a rare disease that affects about 2 every 100,000 people. It is caused by a congenital defect involving the metabolism of amino acids and vitamin B12. This defect causes the malfunctioning of a specific enzyme that makes it impossible for the body to metabolize the proteins derived from food, causing the accumulation in the blood of a substance called methylmalonic acid. The accumulation of methylmalonic acid is extremely harmful for patients that face since the neonatal period acute episodes of neurometabolic decompensation and, in the longer term, end-stage renal failure.
To reduce the toxic accumulation of methylmalonic acid, patients must follow a low-protein diet and take some medications. In severe forms, organ transplantation is increasingly used: liver when there is no kidney failure, kidney or combined liver and kidney when kidney failure is present. The diagnosis is made with biochemical and genetic tests. In Italy, methylmalonic acidemia is included in the diseases subject to mandatory neonatal screening.
THE
STUDY
The results of the international multicentric study coordinated by Dr. Luca Dello Strologo, in charge of kidney transplant follow-up at Bambino Gesù, were presented during the tenth congress of the International Pediatric Transplant Association (IPTA) and will soon be published in a scientific journal. They required the collaboration of 19 large centers between Europe (15) and the United States (4), and the involvement of 83 pediatric patients. These are the largest multicentric case histories collected and analyzed so far. Out of all patients, 26 (31%) had undergone kidney transplantation, 24 (29%) liver transplant, and 33 (40%) both kidney and liver transplantation. The data of the whole cohort was statistically checked to identify the most effective therapeutic solution.
THE
RESULTS
The statistical comparison of data showed that patients undergoing the combined kidney and liver transplant or liver only transplant have lower levels of methylmalonic acid in both blood and urine than those undergoing kidney transplants only. The frequency of metabolic crises as well was reduced in the first two groups.
«Although kidney transplantation was carried out in about 1/3 of cases, and despite being indicated as a possible solution, the data unequivocally demonstrates that it is the therapeutic approach with the worst results» adds Dello Strologo. Liver transplantation as well provided better results than kidney transplantation alone in terms of effectiveness, but in this case, what makes the difference is the precocity of the operation. The median age of liver transplant recipients was in fact significantly lower than the median age of the other two cohorts: 1.8 years compared to 11.1 for kidney transplant recipients and 9.5 for kidney / liver transplant recipients.